The study shows the mean P1NP level in adults with Down syndrome is lower than in controls, with no significant difference in their CTx levels, thus emphasizing a newer paradigm in the treatment of osteoporosis in Down syndrome focused on increasing the amount of bone formation in this population.
Several musculoskeletal abnormalities are associated with Down syndrome, including hypermobility of the joints, as well as low bone density, resulting in frequent fractures of both long bones & vertebral bodies in this population.
Hypermobility is a combined effect of muscle hypotonia and excessive ligamentous laxity. Patellofemoral instability is a common issue, with an estimated incidence of 10–20%, and is generally treated with non-operative modalities, but sometimes may require soft tissue and bony procedures in recurrent symptomatic cases.4 Spinal conditions, such as atlanto-axial or occipital-cervical joint instability with a reported incidence of 10–15% and scoliosis of about 7%, are also some commonly encountered in the Down syndrome population.5-7
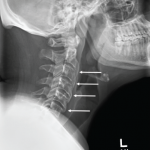
Reports have been made of significant osteoarthritic degenerative changes of the cervical spine with spur formation, narrowing of foramina, narrowing of the disc inner space and osteophyte formation on radiographic review of the C-spine of adults with Down syndrome between 26 and 42 years of age, emphasizing the importance of taking baseline radiographs of the C-spine in all Down syndrome children older than 5 years old and all Down syndrome adults older than 30.8
Foot abnormalities include pes-planus and first ray disorders, including metatarsus primus varus and hallux valgus, the treatment for which always begins with non-operative management, including orthotics or footware modification and surgical options when necessary.6,9,10
Down syndrome also affects the hips, causing slipped capital femoral epiphysis (SCFE), Perthes disease and hip instability.11 The etiology for SCFE in Down syndrome is unknown, although that for Perthes disease and hip instability is related to a multifactorial interplay of bony differences and soft tissue laxity with hypermobility.9,11 The treatment starts with immobilization and, depending on the severity and complexity, surgical interventions.
Arthritis in Down syndrome is less recognized, but as with other arthropathies, can result in chronic disability and functional impairment. The cause for this increased incidence of autoimmune phenomena is unknown. Cases of JIA with Down syndrome were described by Harbir Juj et al., in the Journal of Pediatrics, which stated the prevalence of arthropathy is 8.7/1,000—more than six times higher than JIA in general population.12
Harbir Juj et al. described nine children who had Down syndrome with JIA and a variety of presentations. All responded to different forms of anti-inflammatory medications to some extent. The researchers emphasized that, due to lack of awareness about the occurrence of inflammatory arthritis in Down syndrome, many children had to undergo unnecessary procedures or experienced delayed diagnosis, which led to a few cases of irreversible joint damage. Therefore, it’s very important to address early on any signs of inflammation in a population already at significant risk, to reduce their morbidity burden.