The evidence for EBV as the infectious trigger that causes lupus autoimmunity is much clearer, he said. The high presence of antibodies to EBV nuclear antigen-1 (anti-EBNA-1) in patients’ sera suggests that this viral infection is a key environmental risk factor for later development of lupus.
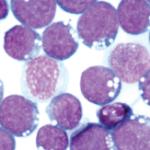
“Lupus patients make a lot of antibodies. It’s dropping out of the solution because it is so concentrated,” Dr. Harley said. Patients have autoantibodies for years before a lupus diagnosis, and can have high levels of these autoantibodies for as many as five years before symptoms show, he said. Those anti-EBNA-1 antibodies bind to lupus-specific autoantigens, such as Ro. Lupus patients often have a 15- to 40-fold increase in Epstein-Barr viral loads, an increased number of EBV-infected B cells, and increased EBV gene expression.
How Genes Come into Play
Somehow, infectious agents interact with an individual’s genetic susceptibility to trigger disease. “Eventually, we will understand the connections between genetics and the environment” in autoimmune diseases, said Dr. Harley.
We still know very little about the genetics of the initiation of disease, said his fellow panelist, V. Michael Holers, MD, head of the Division of Rheumatology at the University of Colorado, Denver. He spoke more about how genes and environment intersect in RA, and referred to a multi-laboratory project to explore the pathogenesis of early RA, the Studies of the Etiology of Rheumatoid Arthritis (SERA), which he co-founded in 2002. SERA’s work includes identifying high-risk populations of individuals who as yet don’t have clinically apparent disease.
“What are the biomarkers and autoantibodies in the evolution of seropositive RA?” Dr. Holers asked. Patients will move through four phases on the road to RA: genetic risk, preclinical autoimmunity, initial signs and symptoms of disease, and then classifiable, clinical disease.
Two biomarkers are important clues in SERA’s findings. Seropositive RA patients exhibit rheumatoid factor (RF) and antibodies to citrullinated protein antigens (ACPA), he said. ACPA is highly specific for RA, and citrullinated proteins are present in the synovium and lungs of patients with RA, sites of inflammation. Using serum data on 83 patients with current RA from the U.S. Department of Defense’s Army-Navy Serum Repository, researchers found signs that ACPA response rapidly expands prior to the development of clinically apparent disease.
“What was the first epitope reactivity, or the original sin” that sets the process of autoimmunity in motion, Dr. Holers said. RA patients often have a robust expansion of inflammatory biomarkers like cytokines and chemokines in their blood before clinically apparent disease. In addition, the effector functions of ACPA evolve as RA develops in the time before the patient is symptomatic, he said. “ACPAs become more potent as the disease progresses, as it picks up more effective aspects of complement.”