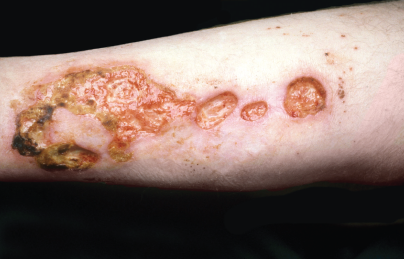
Clinical Photography, Central Manchester University Hospitals NHS Foundation Trust, UK / Science Source
MADRID—During the 2019 European Congress of Rheumatology (EULAR), held June 12–15, speakers addressed the complexity of vasculitis in a Challenges in Clinical Practice session titled, How to Maintain Remission in Vasculitis.
Although vasculitis appears in many varieties, one commonality exists among these related yet distinct conditions: When there is vital organ or systemic involvement, disease progression can be rapid and life threatening. Example: The five-year survival rate for patients in the French Vasculitis Study Group with systemic necrotizing vasculitides, including polyarteritis nodosa (PAN), granulomatosis with polyangiitis (GPA), microscopic polyangiitis (MPA) and eosinophilic granulomatosis with polyangiitis (EGPA), was only 72% through 1980. However, these rates have improved over the years, with 94% of patients in this cohort who were diagnosed after 2010 surviving five years.1 Additionally, research in the U.S. has shown declining in-hospital mortality and mortality due to end-stage renal disease in GPA since the 1990s.2,3
Thus, rheumatologists are left with the difficult task of correctly identifying and treating systemic vasculitis while avoiding the long-term side effects of treatment, such as infection, osteoporosis and negative consequences of corticosteroid therapy. They must also evaluate how best to maintain disease remission in patients.
Treatment Options
Loïc Guillevin, MD, professor of medicine and therapeutics, Hôpital Cochin, Université Paris Descartes, France, began the session. He sought to answer several important questions: What is the ideal induction treatment for anti-neutrophil cytoplasmic antibody (ANCA) associated vasculitis, and what is the effect on maintenance treatment? Do patients with ANCA-associated vasculitis need maintenance treatment, and if so, what treatment? How long should patients with these conditions be treated, and what should long-term treatment entail?
Traditionally, remission in ANCA-associated vasculitis has been achieved with the use of cyclophosphamide and corticosteroids. More recently, rituximab, along with corticosteroids, has become a potential treatment option. In GPA without renal involvement, methotrexate or azathioprine are viable treatment strategies. In some cases, such as EGPA without systemic involvement or signs of poor prognosis, corticosteroids can be used as monotherapy. Prof. Guillevin noted that although remission can be initially achieved with azathioprine, methotrexate or corticosteroid monotherapy, relapse rates are high when treatment is stopped early. Therefore, when immunosuppressants are prescribed to induce remission, a maintenance agent is compulsory.
With regard to cyclophosphamide, the Cyclophosphamide vs. Azathioprine for Early Remission Phase of Vasculitis (CYCAZAREM) trial demonstrated that in patients with generalized vasculitis, withdrawal of cyclophosphamide and substitution of azathioprine after remission did not increase the rate of relapse. This finding indicates that extended treatment with cyclophosphamide is not necessary for maintenance of remission.4 With regard to methotrexate and azathioprine for maintenance of remission in ANCA-associated vasculitis, the two medications were shown to be similar in efficacy in the Wegener’s Granulomatosis–Entretien (WEGENT) trial. But relapse-free survival at 36 months was only 69% in the methotrexate group and 64% in the azathioprine group.5
Thus, attention has turned to the potential of rituximab as a maintenance agent. The Maintenance of Remission Using Rituximab in Systemic ANCA-Associated Vasculitis (MAINRITSAN) trial included 155 patients with newly diagnosed or relapsing GPA, microscopic polyangiitis or renal-limited ANCA-associated vasculitis in complete remission after a cyclophosphamide-glucocorticoid regimen. These patients were randomly assigned to receive 500 mg of rituximab on Days 0 and 14 and at Months 6, 12 and 18 after study entry or daily azathioprine until Month 22. After 28 months of follow-up, 29% of patients in the azathioprine group experienced relapse; only 5% in the rituximab group experienced relapse.6 Prof. Guillevin further noted that after five years of follow-up, relapse-free survival was 72% in rituximab-treated patients and 49% in azathioprine-treated patients.
These findings led to the MAINRITSAN 2 trial, which sought to compare individually tailored (based on trimestrial biological parameter monitoring) with fixed-schedule rituximab reinfusion for remission maintenance of ANCA-associated vasculitis. In this study, patients in the tailored arm received an infusion of 500 mg of rituximab at randomization and then received reinfusion only when CD19+B lymphocytes or ANCA reappeared or the ANCA titer rose markedly. Meanwhile, control patients received a fixed 500 mg infusion of rituximab on Days 0 and 14 post-randomization and then again at six, 12 and 18 months. This study demonstrated that relapse rates did not differ significantly between individually tailored and fixed-schedule rituximab regimens, but individually tailored-arm patients received fewer rituximab infusions.7 Based on these results, Prof. Guillevin concluded that rituximab appears to be safe and effective and that ANCA titer and/or CD19+B lymphocyte count have no clear predictive value.